Viral outbreaks always seem to be at the forefront of America’s collective minds. As a dentist, how should you address people’s concerns? What should you do to ensure you are protecting your patients and staff? Are you up to date with infectious disease outbreaks currently being reported on by CDC?
“Keep Calm and Carry On”
Fortunately, the dental community has focused on infection prevention for years. We have a track record of keeping patients safe from outbreaks that sweep through our communities each year. By following standard best practices, you already slow the spread of infectious diseases like MRSA, Enterovirus 68, and even Ebola.
Here are a few reminders of the infection prevention best practices you are undoubtedly following in your practice today:
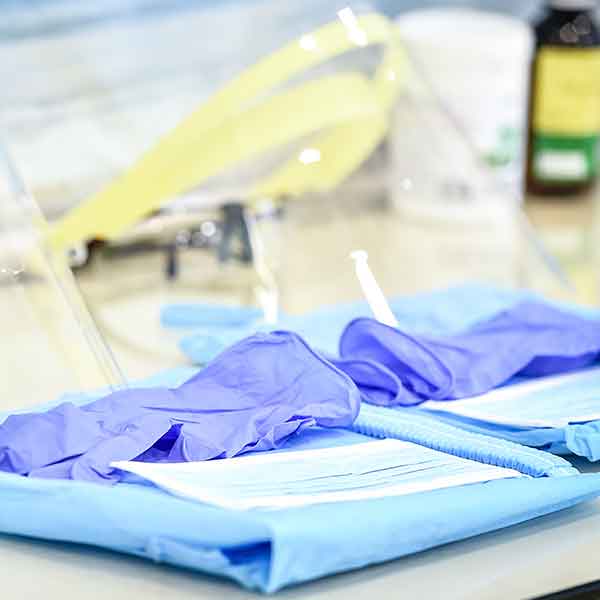
Wearing Personal Protective Equipment (PPE)

The personal protective equipment (PPE) you wear every day—by design—slows the spread of infectious diseases. Take a look at this image (source – New York Times), demonstrating different tiers of protection. Now, note the equipment worn on the left: it looks a lot like the attire you and members of your staff wear every day. Why? Dental procedures create splatter. And so a mask, eye protection, gloves, and gown prevent staff from acquiring infections. It also prevents cross-contamination among patients.
Keep in mind that wearing PPE is important, and its proper removal is also critical. The most common source of infection for healthcare workers is the improper removal of protective equipment, so remind your staff of the order in which they are to remove their PPE:
- Gloves
- Face-Shield
- Gown
- Mask.
Biological Monitoring of Your Autoclaves
Ensuring that your autoclaves are functioning properly and that your instruments are being sterilized is a routine practice in every dental practice. Whether you use in-office testing or send test strips to a third-party laboratory doesn’t matter. You are protecting both staff and patients from the spread of infectious diseases. The test results confirming that your instruments are clean should give you and your patients peace of mind. Showing anxious patients your test log is an excellent way to prove your commitment to cleanliness and to reduce anxiety.
Have a Checklist for Disinfecting Operatories / Common Areas
As you know, infection prevention goes beyond the PPE you wear and instrument sterilization. Getting your operatories and common areas disinfected is just as important. The best way to make ensure your practice achieves the level of cleanliness required is to implement a checklist that integrates the infection prevention protocols like those outlined by OSAP.
Every action on the checklist is itemized. This allows staff to follow step-by-step directions to complete thorough cleanings. A checklist eliminates reliance on staff members’ memories, reducing inadvertent lapses. It will also make auditing for compliance a lot easier: either the operatory is cleaned according to the checklist, or it isn’t. And, you have a record that you (and your staff) followed proper infection prevention procedures.
Conclusion
Following standard dental office infection prevention protocols keep your patients and staff safe from infectious diseases. When we see news stories about virulent disease outbreaks, it’s important to remember: “Keep Calm and Carry On.” With the steps you already take every day, you prevent the spread of infection in your practice.
HealthFirst offers a variety of dental infection control products including spore testing kits, dental unit waterline treatment, surface barrier film, and much more.