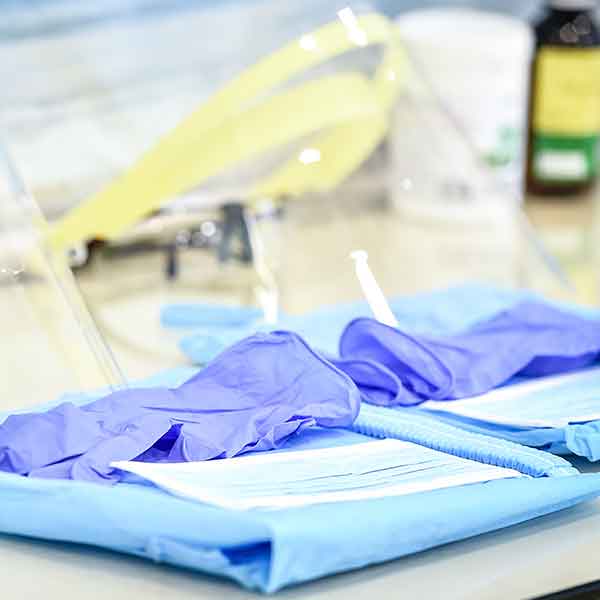
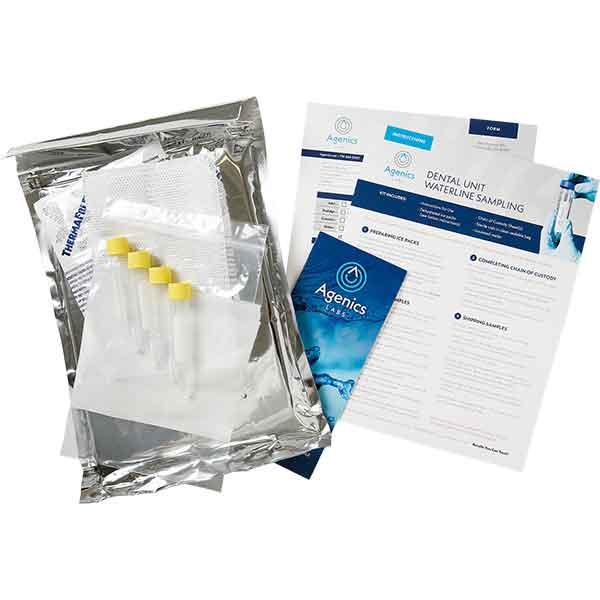
Infection control breaches involve failure to follow recommended/mandated infection control procedures that prevent the transmission of microorganisms and disease. They may not be noticed until an incident occurs.
Common Types of Infection Control Breaches
- Hand washing. In one study in ambulatory care settings, hand hygiene was not properly followed 37% of the time.
- Failure to consistently wear appropriate personal protective equipment (PPE).
- Inappropriate cleaning and disinfection of clinical contact surfaces.
- Failure to adhere to instrument reprocessing instructions and recommendations.
- Re-use of single-use, disposable items.
- Failure to monitor, treat and maintain dental unit waterlines.
- Failure to adhere to the Bloodborne Pathogens (BBP) Standard.
Among documented OSHA violations for dental offices, while noted violations are fortunately relatively uncommon, those related to the BBP Standard top the list. Some can have serious consequences for patients, the healthcare team, and your practice. Between October 2019 and September 2020, OSHA issued 47 citations, conducted 15 inspections, and issued penalties of $111,750 for BBP Standard violations. All of these are preventable, but how?
Here we’ll look at six points and pitfalls related to the BBP Standard.
- Training – Make sure that mandatory training is provided in a timely manner, as required and indicated for individuals at occupational risk for exposure to bloodborne pathogens – initially on assignment and annually. One error is thinking this is sufficient. It’s still required to conduct additional training if changes occur, for example, modifications of tasks or procedures or institution of new tasks or procedures affect the employee’s occupational exposure. This extra training may be limited to addressing the new exposures created.
- Is appropriate PPE always worn? That means PPE that “does not permit blood or other potentially infectious materials to pass through to or reach the employee’s work clothes, street clothes, undergarments, skin, eyes, mouth, or other mucous membranes under normal conditions of use and for the duration of time which the protective equipment will be used.” Essentially, under the Standard, PPE must include appropriate protective clothing, a mask (or respirator), protective eyewear and gloves. ‘Appropriate protective clothing such as, but not limited to, gowns, aprons, lab coats, clinic jackets, or similar outer garments shall be worn in occupational exposure situations. The type and characteristics will depend upon the task and degree of exposure anticipated.’ When there is a risk of sharps injury during non-clinical procedures, puncture-resistant heavy-duty utility gloves are required – including during transportation of instruments. The employer is responsible for making sure appropriate PPE is always worn.
- Hepatitis B Vaccination and Medical Records: Everyone at risk of exposure must be offered this vaccination series within 10 days of assignment, after first being educated on the vaccine, vaccination and benefits of being vaccinated. Either a 2- or 3-dose series is acceptable. Individuals must first be educated on BBP, the benefits of vaccination, and offered the vaccine for free and at a convenient time. If individuals refuse vaccination, they must sign a declination form – and may change their mind later. The signed declination form must then be kept as part of the individual’s confidential medical records in their personnel file. One potential pitfall is the length of time for which medical records must be kept. In accordance with 29 CFR 1910.1020, the employer shall maintain medical records for at least the duration of employment plus 30 years.
- Are engineering controls, including safer medical devices, being identified, considered and used? The employer must obtain input on the selection of effective engineering and work practice controls from ‘non-managerial employees responsible for direct patient care who are potentially exposed to injuries from contaminated sharps.’ It is required to ‘Document annually consideration and implementation of appropriate commercially available and effective safer medical devices designed to eliminate or minimize occupational exposure. An example would be a self-sheathing needle, or a needleless device. OSHA does not mandate a specific brand/device. Engineering controls being used must be documented.
- Is regulated medical waste being properly handled? Proper use and disposal of appropriate sharps containers is required – the container must be both closed and sealed for disposal when the fill line is reached. Contaminated laundry must be red-bagged and sent to a professional laundry or laundered on the premises. It is not permissible to take it home for laundering. If items are wet, the container/bag must be leak-proof. Other regulated medical waste must also be red-bagged. Extracted teeth containing amalgam must be placed in a contact waste amalgam container, not red-bagged.
- Do you have a thorough, updated written exposure control plan for your office? The written exposure control plan needs to be reviewed and updated at least annually and ‘whenever necessary to reflect new or modified tasks and procedures which affect occupational exposure and to reflect new or revised employee positions with occupational exposure.’ IT must also be accessible for workers. A sample written exposure control plan with the required elements and an explanation of what must be included can be found on OSHA’s website.
Last but not least, make sure you have a post-exposure management program in place and documented. Always remember: Safety First and Be Prepared!
Fiona M. Collins, BDS, MBA, MA
Dr. Collins is a recognized dental infection control expert and a national and international speaker and author. Her topics include infection control and OSHA, dental caries, xerostomia, oral disease prevention, vaping and tobacco cessation. During her career, Fiona has lived and worked in five countries. Dr. Collins graduated as a general dentist from the University of Glasgow in Scotland and holds an MBA and an MA from Boston University.
Reference:
Association for Professionals in Infection Control and Epidemiology (APIC), April 11, 2016. Handwashing gets skipped a third of the time in outpatient healthcare: study. Available at: https://www.oralhealthgroup.com/infection-control/
OSHA. Model Exposure Control Program:
https://www.osha.gov/Publications/osha3186.html
OSHA. NAICS Code: 6212 Offices of Dentists. Available at: https://www.osha.gov/pls/imis/citedstandard.naics?p_esize=&p_state=FEFederal&p_naics=6212
OSHA Regulations (Standards – 29 CFR) Bloodborne Pathogens. – 1910.1030.
Page 10 and 11 of 22, section (d)(4)(iv).